Single Tooth Implants- A Complete Clinical Guide by Dr.Ankur Jain, Best Implantologist Gurgaon
Single Tooth Implants- A Complete Clinical Guide by Dr.Ankur Jain, Best Implantologist Gurgaon
🦷 Single Tooth Implants: A Complete Clinical Guide to Root Replacement, Osseointegration & Long-Term Bone Health
Published by White Smile Dental Care — Gurgaon & Delhi
Tooth loss is rarely just a cosmetic concern. Even the absence of a single tooth initiates a cascade of biological, structural, and functional changes that can progressively compromise oral health, facial integrity, and adjacent dentition.
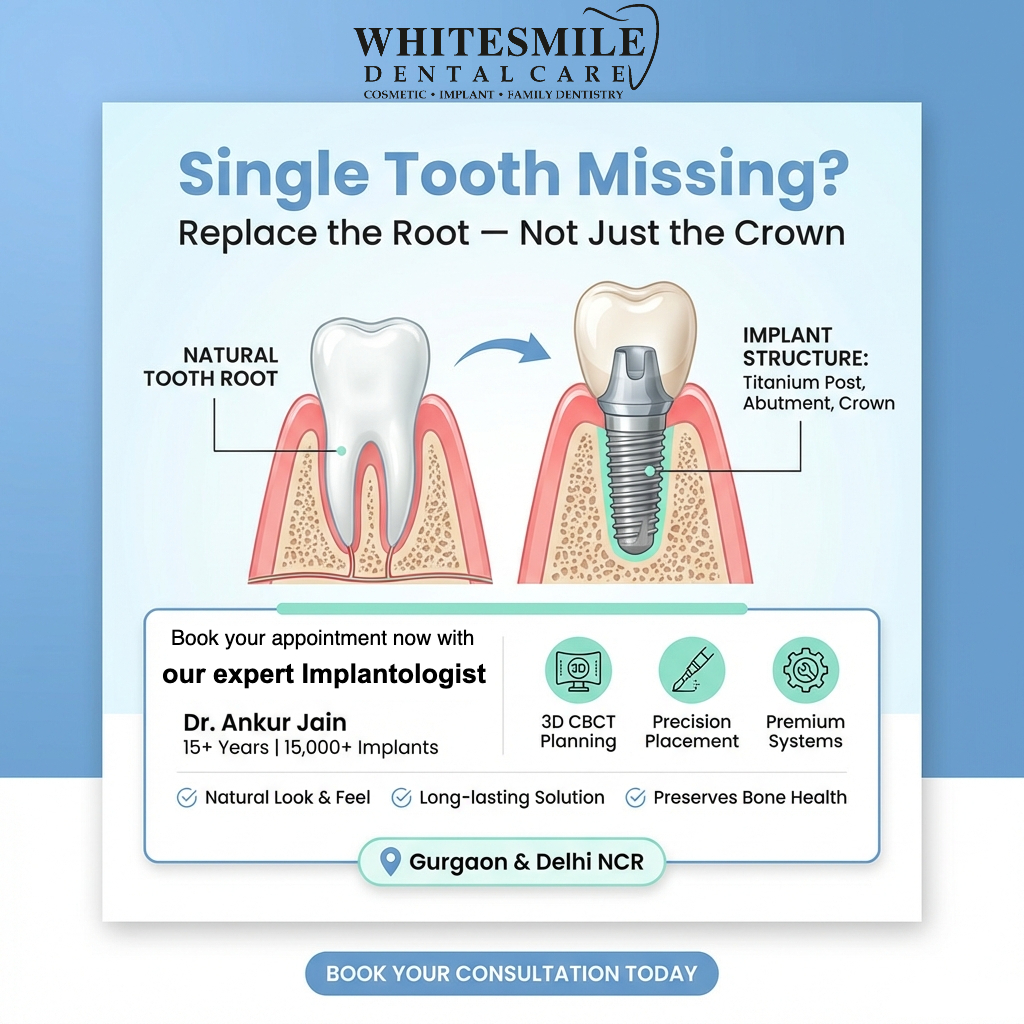
A single tooth implant is not merely a replacement for what is visible; it is a precise biological reconstruction of the missing root and crown. In modern dentistry, it is widely regarded as the most anatomically accurate and long-term stable method of tooth replacement available today. 🦷✨
At White Smile Dental Care, implant dentistry is practiced as a specialized clinical discipline. Every implant case is guided by advanced diagnostics, biomechanical planning, and individualized surgical execution. his guide explains, in clinical detail, how single tooth implants work from titanium root integration to long-term bone maintenance and what patients in Delhi NCR should understand about the procedure, healing timeline, and overall treatment value.
This comprehensive guide explains:
✔️ How single tooth implants work
✔️ Why root replacement is biologically critical
✔️ How osseointegration preserves jawbone
✔️ What patients in Delhi Gurgaon should expect
✔️ Cost considerations and long-term value
📚 Table of Contents
1️⃣ Understanding Single Tooth Implants
2️⃣ The Biology of Tooth Loss
3️⃣ Implant Anatomy: Components Explained
4️⃣ Step-by-Step Implant Procedure
5️⃣ Osseointegration: The Science Behind Stability
6️⃣ Preserving Jawbone Integrity
7️⃣ Functional & Aesthetic Outcomes
8️⃣ Single Tooth Implant Cost in Gurgaon & Delhi
9️⃣ Why Clinical Expertise Matters
🔟 References
Frequently Asked Questions
1️⃣ Understanding Single Tooth Implants 🦷
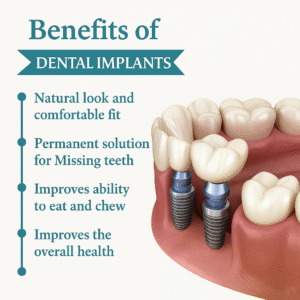
A single tooth implant is a fixed, permanent prosthetic solution designed to replace one missing tooth in its entirety both the visible crown and the underlying root. It is widely regarded as the gold standard for single tooth replacement, not merely for aesthetic reasons, but because it is the only restorative option that replicates the full anatomical structure of a natural tooth.
A single tooth implant is a fixed, permanent restoration designed to replace one missing tooth including both:
• The visible crown 👑
• The underlying root structure
Unlike conventional fixed bridges, which depend on the reduction of healthy adjacent teeth for support, or removable partial dentures, which rest on soft tissue and neighboring teeth, a single tooth implant is entirely self-supporting. It is anchored within the jawbone itself, functioning in a manner biomechanically equivalent to a natural tooth root.
❌ Dental bridges (which depend on shaving healthy neighboring teeth)
❌ Removable dentures (which rest on gums and can move)
An implant is:
✅ Independent
✅ Self-supporting
✅ Anchored directly into bone
✅ Biomechanically similar to a natural tooth
According to the American Academy of Implant Dentistry, dental implants most closely replicate the anatomy and function of natural teeth among all replacement options.
2️⃣ The Biology of Tooth Loss: Why the Root Matters 🧬
To appreciate why single tooth implants offer such a significant biological advantage, it is essential to understand what occurs in the jawbone following the extraction of a tooth. The consequences of an unreplaced root are progressive, cumulative, and in many cases, irreversible without surgical intervention.
The alveolar bone- the portion of the jaw that houses and supports tooth roots. It is a dynamic, metabolically active tissue. Its density and volume are maintained through a process called functional loading: the mechanical stimulation transmitted through tooth roots during biting, chewing, and other oral functions. When a root is removed, this stimulation ceases entirely. In the absence of functional load, the body interprets the bone as unnecessary and initiates a process of resorption, gradually breaking down and reabsorbing the bone tissue.
⏳ Timeline of Bone Resorption after tooth loss:
• Within the first 3 months: Approximately 40–60% of alveolar bone width may be lost.
• Within the first year: Bone height in the extraction socket can reduce significantly.
• Over several years: Continued resorption progressively flattens the alveolar ridge, altering facial contours and making future implant placement more complex.
Research from the National Institutes of Health confirms that dental implants, by transmitting occlusal forces into the alveolar bone, are effective in preserving bone volume in a manner that bridges and dentures cannot replicate. This biological reality fundamentally positions single tooth implants not merely as a cosmetic solution, but as a preventive medical intervention.
Secondary Consequences of an Unreplaced Tooth
• Mesial drift: Adjacent teeth gradually migrate into the empty space, disrupting arch alignment.
• Over-eruption: The opposing tooth in the arch may erupt downward or upward into the gap, compromising bite balance.
• Increased caries risk: Shifted teeth create new areas of difficult oral hygiene access.
• Temporomandibular joint (TMJ) strain: Bite imbalances can create asymmetric loading of the jaw joint, potentially causing discomfort or dysfunction.
When a tooth is lost, the problem is not just visible space, it is the loss of functional stimulation to the jawbone. The alveolar bone is a metabolically active structure that depends on mechanical loading from tooth roots. Once the root is removed:
⚠️ Bone stimulation stops
⚠️ Bone begins to resorb (shrink)
⚠️ Facial contours gradually change
Research from the National Institutes of Health confirms that implants preserve bone by transmitting occlusal forces directly into the jaw — something bridges and dentures cannot achieve.
Secondary Consequences of an Unreplaced Tooth
• ➡️ Adjacent teeth drift into the gap
• ⬆️ Opposing tooth over-erupts
• 🦠 Increased cavity risk
• 😣 Bite imbalance & TMJ strain
Replacing the root is not cosmetic; it is preventive medicine.
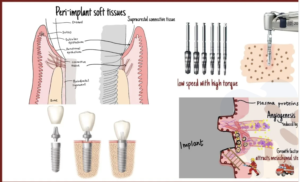
3️⃣ Implant Anatomy: Understanding the Three Components 🔬
A single tooth implant system consists of three precisely engineered components:
🟢 1. Implant Fixture (Root Analog)
The implant fixture is a precision-machined titanium post, typically threaded, that is surgically placed into the jawbone. Titanium is used because of its exceptional biocompatibility; it provokes minimal immune response and uniquely allows bone tissue to grow directly onto and into its surface, a process known as osseointegration. The implant surface is typically treated (acid-etched, sandblasted, or coated) to enhance bone cell attachment and accelerate integration. Fixture lengths and diameters vary according to the specific bone anatomy of the patient.
🟢 2. Abutment (Connector)
The abutment is the intermediary component that connects the implant fixture below the gumline to the visible crown above it. It is placed after the implant has fully integrated with the bone. Abutments are available in various materials including titanium, zirconia, and gold alloy. Zirconia abutments are frequently preferred in the anterior (front) aesthetic zone due to their tooth-colored appearance and minimal gum discoloration.
• Connects implant to crown
• Materials: Titanium, Zirconia, Gold alloy
• Zirconia preferred for front teeth for aesthetics
🟢 3. Crown (Visible Tooth)
The crown is the visible, tooth-shaped restoration that sits atop the abutment. It is custom-fabricated using digital impressions or traditional molds to match the shape, size, and shade of the surrounding natural dentition. Crowns are most commonly fabricated in zirconia or porcelain-fused-to-metal (PFM) and are permanently cemented or screw-retained to the abutment.
• Custom fabricated using digital scans
• Materials: Zirconia or PFM
• Cemented or screw-retained
• Designed for precise occlusion and shade match 🎨
4️⃣ Step-by-Step: Implant Procedure at White Smile Dental Care 🏥
At White Smile Dental Care, implant placement follows a strict evidence-based protocol that prioritizes precision, patient safety, and predictable long-term outcomes. Each phase is deliberate, and no step is omitted or accelerated without clinical justification.
🩺 Phase 1: Comprehensive Evaluation
• Medical & dental history
• 3D CBCT scan/ OPG
• Bone density & nerve mapping
• Occlusal analysis
The process begins with a thorough clinical assessment including a detailed medical and dental history. Radiographic imaging typically cone beam computed tomography (CBCT) or OPG is used to create a three-dimensional model of the jawbone, enabling precise measurement of bone volume, density, and the positions of critical anatomical structures such as the inferior alveolar nerve (mandible) or maxillary sinus (upper jaw). This data is used to plan implant positioning, angulation, and depth prior to any surgical intervention.
📋 Phase 2: Personalized Treatment Planning
• Implant system selection
• Timeline discussion
• Sedation options
• Transparent cost breakdown
No one-size-fits-all treatment protocols. ❌
Based on the evaluation findings, a personalized treatment plan is formulated and discussed with the patient. This includes implant brand selection, expected timelines, sedation options, and cost transparency. At White Smile Dental Care, patients are never presented with a one-size-fits-all protocol.
🔩 Phase 3: Surgical Implant Placement
• Local anesthesia (pain-free)
• Precise osteotomy preparation
• Implant placed with torque control
• Sutures placed
⏱ Duration: 45–90 minutes
The surgical procedure is performed under local anesthesia and, when indicated, sedation. A small incision is made in the gingival tissue to access the bone. A precisely calibrated sequence of implant drills creates the osteotomy (bone channel) to the required depth and diameter. The titanium implant fixture is then placed with controlled torque to achieve primary stability. Sutures are placed to close the site. The procedure typically takes 45–90 minutes for a single implant and is well-tolerated by most patients.
🦴 Phase 4: Osseointegration (8–16 Weeks)
Bone cells attach and mature around implant surface.
Healing time varies based on:
• Bone density
• Systemic health
• Implant surface
• Smoking status
Following surgical placement, the implant enters a critical healing period during which bone cells progressively bond with the implant surface. This phase typically spans 8 to 16 weeks, depending on the quality and density of the patient’s bone, the implant surface technology used, and individual healing capacity. Patients are monitored clinically and radiographically throughout this period. Dr.Ankur Jain is an expert for immediate loading as well but he takes that call on the condition of the bone of the patient.
🔗 Phase 5: Abutment Placement
• Minor second-stage procedure (if needed)
• Gum contouring around abutment
Once osseointegration is confirmed, a minor second procedure is performed to expose the top of the implant (if submerged) and attach the abutment. In cases of simultaneous abutment placement during the initial surgery (one-stage protocol), this step is omitted. The gingival tissues are then allowed to heal and contour naturally around the abutment.
👑 Phase 6: Crown Placement
• Digital impressions
• Lab fabrication
• Occlusal adjustments
• Final cementation
Impressions or digital scans of the abutment and surrounding teeth are used to fabricate the custom crown in the laboratory. Once complete, the crown is fitted, adjusted for occlusal contact, and permanently cemented or screw-retained. The restoration is now clinically complete.
Smile restored. Function restored. Confidence restored. 😊

5️⃣ Osseointegration: The Science of Stability 🧬
Osseointegration is the biological cornerstone of implant dentistry. First described by Professor Per-Ingvar Brånemark in the 1960s, it refers to the direct structural and functional connection between living bone tissue and the surface of a load-bearing implant, without any intervening soft tissue layer.
Following implant placement, a biological sequence unfolds: blood clot formation at the implant-bone interface is followed by the migration of bone-forming cells (osteoblasts) to the implant surface. Over weeks, woven bone gradually matures into dense lamellar bone that physically interlocks with the micro-textured implant surface. This creates a bond of remarkable mechanical strength.
Factors that influence osseointegration quality:
• Bone density and volume at the implant site.
• Implant surface topography; micro-roughened surfaces significantly accelerate bone cell attachment.
• Surgical technique; minimizing heat generation during drilling protects bone vitality.
• Systemic health; conditions such as uncontrolled diabetes or smoking can impair the process.
• Post-operative load management; premature loading before adequate integration can compromise stability.
Long-term clinical studies consistently report survival rates exceeding 95% for properly planned and executed single tooth implants over periods of 10 years and beyond. At White Smile Dental Care, implant brands with established clinical longevity records are exclusively used, and every case is supported by pre-surgical CBCT / OPG analysis to optimize integration outcomes.
Sequence:
🩸 Blood clot formation
🦴 Osteoblast migration
🔬 Woven bone formation
🏗 Mature lamellar bone development
6️⃣ Preserving Jawbone Integrity 🦴
The ability to preserve jawbone volume is one of the most clinically significant advantages single tooth implants offer over all other restorative alternatives. This is not a secondary benefit, it is a primary medical rationale for implant placement.
Studies published in the Journal of Oral Implantology confirm that maintaining functional load at the bone level which only implants provide directly reduces the rate and extent of alveolar bone resorption,
In practical terms, this means that patients who receive implants promptly after tooth loss preserve facial volume and bone height that would otherwise deteriorate over years.
What bridges and dentures cannot provide:
• Dental bridges span the gap left by a missing tooth but leave the underlying alveolar bone entirely without stimulation. Bone loss beneath a bridge continues unimpeded.
• Removable partial dentures rest on the gum surface and exert compressive pressure on soft tissue rather than functional load through bone. This may actually accelerate resorption in some patients.
• Neither bridges nor dentures halt the progressive structural changes caused by missing roots, only implants address the problem at its source.
In cases where significant bone loss has already occurred prior to implant evaluation, bone grafting procedures may be required to restore adequate bone volume before implant placement. At White Smile Dental Care our expert implatologist Dr.Ankur Jain (with an experience of placing 15000+ implants) assess bone quantity and quality comprehensively at the initial diagnostic stage, ensuring that every patient receives a transparent picture of their clinical situation and treatment options.
What Alternatives Cannot Do:
❌ Bridges do not stimulate bone
❌ Dentures compress soft tissue
❌ Neither prevents progressive resorption
Only implants address the root-level cause of bone deterioration.
7️⃣ Long-Term Functional & Aesthetic Outcomes ✨
When properly planned and executed, a single tooth implant restoration offers outcomes that closely parallel the natural dentition in both function and appearance and in many respects surpasses conventional restorations in durability and long-term stability.
Functional outcomes:
• Restoration of chewing efficiency to near-natural levels, enabling patients to resume a full, unrestricted diet.
• Stable bite alignment preserved by the implant’s resistance to the movement of adjacent and opposing teeth.
• Speech clarity restored particularly important in anterior (front tooth) replacement cases.
• Independent cleaning maintained, as the implant is flossed and brushed like a natural tooth with no additional prosthetic hygiene complexity.
Aesthetic outcomes:
• Custom-shaded, custom-shaped crowns fabricated to match the surrounding dentition precisely.
• Healthy gingival (gum) architecture maintained around the implant, replicating natural tooth emergence profile.
• Preservation of facial volume due to maintained bone height, preventing the sunken appearance associated with long-term tooth loss.
• No visible metal margins, clasps, or prosthetic components in the smile zone.
Implants integrate into your smile ; not sit on top of it.
8️⃣ Single Tooth Implant Cost in Gurgaon & Delhi 💰
A common and entirely understandable concern among patients evaluating implant treatment is cost. The single tooth implant cost in Gurgaon and Delhi varies depending on a range of clinical and non-clinical factors, and understanding these variables helps patients evaluate the treatment in its proper context not merely as a price point, but as a long-term clinical investment.
Factors influencing implant cost in Delhi NCR:
• Implant brand and surface technology: Premium implant systems with established clinical track records (such as Straumann, Nobel Biocare, or Osstem) involve higher material costs but offer superior long-term predictability.
• Diagnostic workup: CBCT scanning /OPG and comprehensive pre-surgical assessment add to upfront cost but are non-negotiable from a clinical safety and outcomes perspective.
• Abutment and crown material: Zirconia abutments and all-ceramic crowns are more expensive than metal alternatives but offer superior aesthetics and biocompatibility.
• Surgical complexity: Cases requiring bone grafting, sinus lift, or other augmentation procedures prior to implant placement involve additional clinical time and material costs.
• Clinician expertise and clinic infrastructure: Experienced implantologists with advanced training and modern surgical environments appropriately command higher fees.
Long-term cost comparison:
While the initial dental implant cost in India may appear higher than a conventional bridge or denture, the long-term financial calculus typically favors implants significantly. Dental bridges generally require replacement every 7–10 years and involve the irreversible modification of adjacent healthy teeth. Dentures require periodic relining and replacement. Implants, with appropriate maintenance, can last several decades. Research from Harvard School of Dental Medicine supports the cost-effectiveness of dental implants over a 10–20-year horizon relative to alternative restorations. When evaluated over a patient’s lifetime, implants frequently represent the most economically rational option.
At White Smile Dental Care, patients receive a fully transparent, itemized treatment estimate prior to commencing any procedure. There are no hidden costs, and all clinical decisions are made in the patient’s best interest rather than driven by commercial considerations.
At White Smile Dental Care, all pricing is transparent and itemized.
9️⃣ Why Expertise Defines Implant Success 🎯
Implant dentistry is not a standardized procedure that yields uniform results regardless of who performs it. The International Team for Implantology (ITI) explicitly recognizes clinician expertise as one of the primary determinants of implant success rates. The following clinical factors, all directly within the control of the treating team, significantly influence outcomes:
• Pre-surgical CBCT analysis: Enables accurate 3D bone assessment, avoiding nerve damage, sinus perforation, or sub-optimal implant positioning.
• Surgical guide use: Digitally fabricated surgical guides allow for precise, planned implant placement that aligns with the prosthetic goal.
• Implant torque control: Achieving correct primary stability during placement without over-compressing bone requires refined surgical technique.
• Sterilization and infection control: Adherence to surgical sterilization standards directly affects post-operative infection rates and integration outcomes.
• Post-operative monitoring: Regular follow-up at defined intervals allows early identification and management of any complications.
• Prosthetic precision: Crown fabrication that achieves accurate occlusal contact prevents overloading of the implant and surrounding bone.
White Smile Dental Care’s implant team in Gurgaon and Delhi combines advanced implantology training with evidence-based protocols and modern surgical infrastructure.
Critical success factors include:
• 3D CBCT planning
• Surgical guide precision
• Controlled torque placement
• Strict sterilization
• Accurate occlusal calibration
• Structured follow-up
Implant dentistry is precision medicine ; not a commodity procedure.

🔟 References
-
American Academy of Implant Dentistry
-
National Institutes of Health
-
Journal of Oral Implantology
-
International Journal of Oral Implantology
-
Harvard School of Dental Medicine
-
International Team for Implantology
1️⃣1️⃣ Frequently Asked Questions ❓
❓ Is the procedure painful?
No. Local anesthesia ensures comfort. Most patients report less discomfort than a tooth extraction. Mild soreness may last 2–4 days.
❓ How long does a single tooth implant last?
20–30 years or more with proper hygiene. Many last a lifetime. Crown may need replacement after 15–20 years.
❓ Am I a suitable candidate?
Most healthy adults qualify. Conditions like uncontrolled diabetes or heavy smoking may require additional management.
❓ Is it worth the investment?
Yes, biologically, functionally, and financially over time.